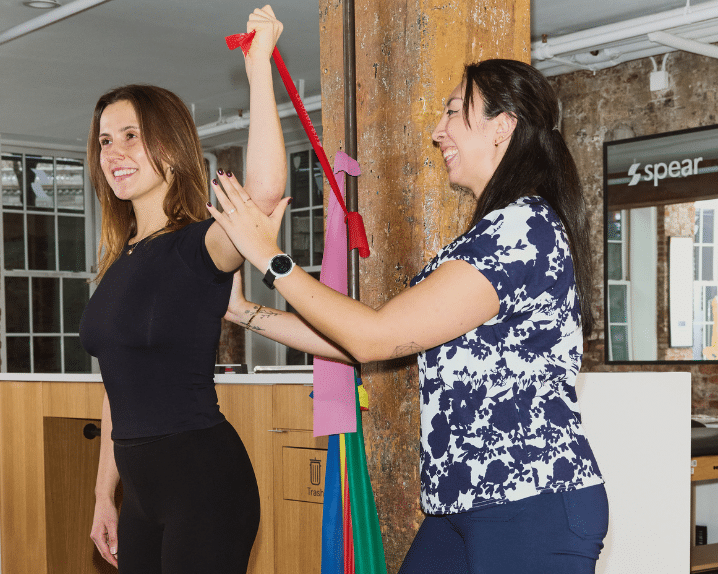- Locations
- Take a tour
- Explore providers
- Services
- Ready to get started?From pediatrics to geriatrics, hand therapy to TMJ, golf swing analysis to women’s health, and more, we take the time to understand your needs and match you with one of our top-rated therapists to create a personalized program that perfectly aligns with your unique goals.View all
Popular
Physical therapy
Popular
Occupational therapy
- About
- Careers